Denial management in medical billing is the systematic process of investigating, resolving, and preventing denied insurance claims. Its goal is to maximize provider revenue by identifying root causes of denials, correcting claims, filing appeals, and implementing preventive measures to minimize future financial losses.
When integrated into a broader revenue cycle management strategy, effective denial management strengthens cash flow, reduces administrative burden, and improves the financial stability of any practice.
This guide covers everything you need to know about denial management in 2026, from definitions and root causes to prevention strategies and appeals workflows.
Understanding what a denial actually means is the first step toward managing it effectively. A denial occurs when a payer refuses to reimburse a submitted claim, either partially or in full. This is different from a rejection, which happens before a claim enters the adjudication process due to a technical or formatting error.
Read more; Top 10 denial codes in medical billing
A rejected claim never reaches the payer's review system. It is returned immediately due to missing or invalid data, such as an incorrect patient ID or a formatting error.
A denied claim, by contrast, has been received and reviewed by the payer but determined ineligible for payment based on coverage, coding, documentation, or policy grounds.
Rejections are corrected and resubmitted quickly, while denials require investigation, documentation, and often a formal appeal.
The financial consequences of unmanaged denials are significant. Industry estimates suggest that up to 65 percent of denied claims are never reworked or appealed, representing a direct and permanent loss of revenue.
Beyond the financial impact, denials increase administrative workload, extend accounts receivable days, and create compliance risks when patterns go undetected.
Denial management in healthcare refers to the end-to-end workflow that healthcare organizations use to track, analyze, resolve, and prevent claim denials. It is not simply a back-end billing function.
It is a proactive, data-driven process that touches every stage of the revenue cycle, from patient registration and insurance verification to medical coding services, claims processing, and payment posting. By ensuring coding accuracy and compliance, medical coding services play a crucial role in reducing denials and improving reimbursement outcomes.
The stakes have increased significantly heading into 2026. Initial claim denial rates reached approximately 11.8 percent in 2024, and payer scrutiny continues to intensify.
Value-based care models, evolving payer policies, and growing documentation requirements have made denial prevention a strategic priority rather than an operational afterthought. Practices that invest in structured denial management consistently outperform those that rely on reactive, case-by-case resolution.
Read more; Top 10 benefits of outsourcing denial management services
Denial management directly affects every key revenue cycle metric, including clean claim rate, days in accounts receivable, net collection rate, and cost to collect. A well-functioning denial management program does not just recover lost revenue — it improves the efficiency of the entire billing operation.
The denial process in medical billing follows a defined sequence of steps. Skipping or rushing any step increases the risk of permanent revenue loss.
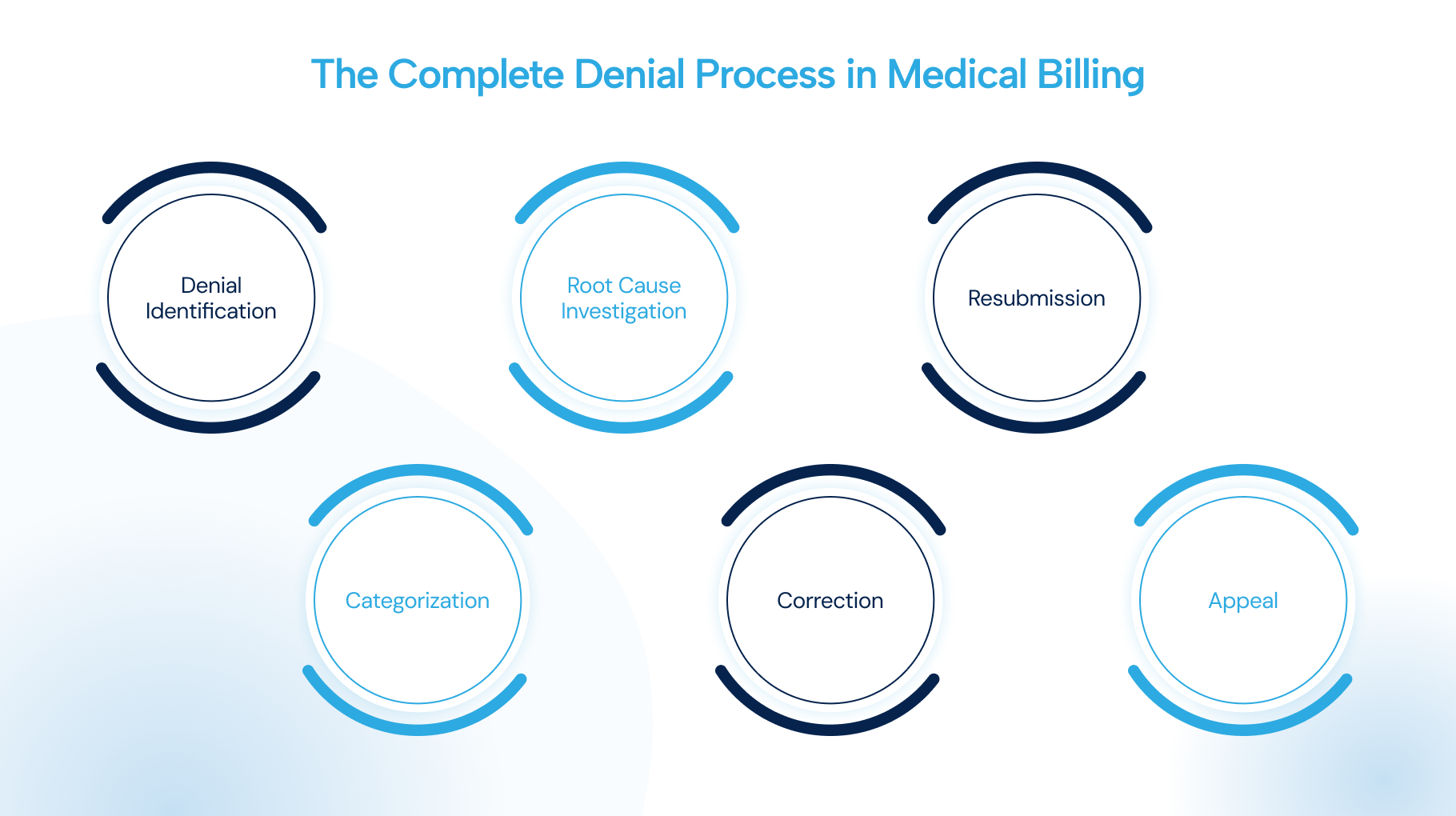
Denial Identification: The billing team identifies a denied claim through the payer's remittance advice, explanation of benefits, or practice management system alerts.
Categorization: The denial is categorized by type, such as clinical, administrative, technical, or eligibility-related, to determine the appropriate response pathway.
Root Cause Investigation: The team reviews the original claim, clinical documentation, payer policy, and coding to identify the specific reason for the denial.
Correction: Based on the root cause, the claim is corrected. This may involve updating codes, adding missing documentation, or obtaining a required authorization retroactively.
Resubmission: The corrected claim is resubmitted electronically within the payer's timely filing window, with all supporting documentation attached.
Appeal: If the payer upholds the denial after resubmission, a formal appeal is filed with a written argument, clinical evidence, and payer policy references to support the claim.
Each step requires clear documentation and tracking to ensure no denied claim falls through the cracks.
Resolving individual denials addresses symptoms. Denial analysis in medical billing addresses the underlying causes that generate denials repeatedly across the revenue cycle.
Without systematic analysis, the same errors recur month after month, draining revenue and increasing administrative costs. Denial analysis identifies patterns across claim types, payers, providers, and departments, allowing practices to intervene at the source rather than managing the consequences.
The most frequent denial categories fall into five areas: coding errors, eligibility issues, authorization gaps, documentation deficiencies, and timely filing failures. Each category has a different root cause and requires a targeted corrective strategy.
Modern billing software and revenue cycle platforms provide dashboards that track denial rates by category, payer, and provider. These insights allow billing leaders to prioritize high-impact interventions, set measurable improvement targets, and report progress to practice leadership with data-backed clarity.
Recurring denials often indicate systemic problems. These may include:
Repeated coding inconsistencies
Missing prior authorizations
Incorrect patient eligibility verification
Timely filing failures
When patterns are ignored, denial rates increase.
The most effective medical billing denial solutions focus on prevention rather than recovery. Stopping denials before they occur is always more efficient than resolving them after the fact.
Insurance eligibility and benefits should be verified at the time of scheduling and again at check-in. Real-time eligibility tools catch coverage gaps, inactive policies, and coordination of benefits issues before a claim is ever submitted.
Specialty-trained coders who understand payer-specific rules significantly reduce coding-related denials. Regular documentation audits ensure that clinical notes support billed services and meet medical necessity standards. Feedback loops between coders and clinicians reinforce good documentation habits over time.
Automated claim scrubbing tools identify errors before submission, reducing the volume of preventable denials. Equally important is investing in ongoing staff training, particularly when payer rules, coding standards, or billing software change. Well-trained teams catch issues earlier and resolve them faster.
Tracking key performance indicators such as denial rate, first-pass acceptance rate, and days in accounts receivable gives practices the visibility needed to measure improvement and identify emerging problem areas before they escalate.
Not every denial can be prevented, and not every denied claim should be written off. A structured appeals process is essential for recovering revenue that would otherwise be lost permanently.
A claim should be appealed when the denial reason is disputable, when documentation supports medical necessity, or when the payer's decision appears inconsistent with the terms of the provider's contract. High-dollar claims should always be reviewed for appeal potential before any write-off decision is made.
Read more; Mental health billing denials and appeals
A strong appeal includes a clear written argument that addresses the specific denial reason, relevant clinical documentation such as physician notes and lab results, references to payer policy or coverage guidelines that support payment, and any corrected coding or authorization documentation if applicable.
Most payers require appeals to be filed within 30 to 180 days of the denial date, depending on the payer and plan type. Missing these windows eliminates the right to appeal entirely.
Practices should maintain a dedicated appeals tracking system that logs submission dates, payer responses, and escalation timelines to ensure every appeal is pursued to resolution.
Denial management in medical billing is no longer a back-office function — it is a core component of financial strategy in 2026. As payer requirements grow more complex and denial rates continue to rise, practices that build proactive, data-driven denial management programs will recover more revenue, reduce administrative costs, and maintain stronger cash flow.
The path forward requires structured workflows, accurate medical coding, front-end verification, and consistent denial analysis to identify and eliminate recurring problems at their source.
What is the difference between a denial and a rejection in medical billing?
A rejection occurs before payer review due to a technical error, such as a missing field or invalid code. A denial occurs after the payer has reviewed the claim and determined it is not eligible for payment. Rejections are corrected quickly, while denials require investigation and often a formal appeal.
What is an acceptable denial rate for a medical practice?
Industry benchmarks suggest a clean claim denial rate of 5 percent or below is considered strong performance. Rates above 10 percent indicate systemic issues in coding, documentation, or front-end verification that require immediate attention.
How can practices reduce claim denials?
The most effective strategies include real-time eligibility verification, accurate medical coding, pre-submission claim scrubbing, regular documentation audits, and consistent staff training on payer-specific requirements.
How long does the appeals process typically take?
Appeals timelines vary by payer. Most commercial payers respond within 30 to 60 days of receiving an appeal. Medicare and Medicaid appeals can take longer depending on the level of appeal and whether a hearing is requested.
What tools are most effective for denial tracking and management?
Practice management systems with built-in denial dashboards, automated claim scrubbing tools, and revenue cycle analytics platforms provide the visibility needed to track denial trends, measure recovery rates, and prioritize high-impact interventions.
Optimize billing, claims and collections with expert RCM support let our professionals handle the process so you can focus on patient care.
